SMOKING AND RISK OF SURGERY
Smokers do less well after surgery than non-smokers.A recent study showed that smokers were 38% more likely to die after surgery than patients who had never smoked. Smokers had twice the normal risk of getting pneumonia and were 80% more likely to have a heart attack, 70% more likely to have a stroke, and 30% more likely to have a postoperative infection compared to non-smokers (Turan 2011).
BREATHING PROBLEMS
Tobacco smoke damages the lining of the lung, reducing its ability to clear waste particles and secretions, which can result in pneumonia. Cigarette smoking reduces the ability of the immune system to fight infection.
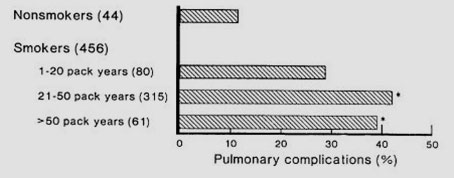
Smokers have about a 40% chance of having breathing problems after surgery, compared to 11% in non-smokers.
HEART PROBLEMS
Nicotine in tobacco smoke acts on the nervous system to cause high blood pressure and a faster heart rate, so the heart has to work harder. The carbon monoxide in cigarette smoke combines with haemoglobin in the blood so that it is less able to deliver oxygen to the heart and other tissues. Anesthesiologists see signs of heart stress on the ECG monitor more often in smokers than in non-smokers, and smokers are 80% more likely to have a heart attack after surgery.
WOUND INFECTIONS
In many studies, wound infections were more common in smokers than in non-smokers.Smokers are up to six times more likely to have a wound infection after surgery (Sorensen 2003).
FAILURE OF VASCULAR FLAPS
Smokers heal less well, especially in plastic procedures requiring a flap of tissue to repair the wound, where they have over twice the risk of the flap dying compared to non-smokers (Chang, 2002). Some plastic surgeons will not perform some types of flaps for their patients unless they stop smoking, as otherwise the risk of complications is too high. In one study, the risk of the flap dying was halved if patients stopped smoking before surgery, but was still four times the risk of patients who had never smoked (Padubidri 2001).
POOR BONE HEALING
Smoking interferes with the cells needed to repair bone, so that smokers are less able to heal after a broken bone or after back surgery.
In back surgery, the failure rate for spinal fusion is twice as high in smokers as in non-smokers (Glassman, 2000).
The bad effects of smoking last for a long time. Smokers have a worse outcome one year after a knee ligament repair. They have more pain, poorer knee function, and are less likely to be able to return to sports that non-smokers (Karim 2006).
VASCULAR SURGERY
If patients continue to smoke, their underlying condition will get worse. This is most noticeable in patients who need surgery to improve the blood flow to their heart or legs. The problem was usually caused by smoking, and if they continue to smoke after surgery they will lose the benefit of the operation and have to have further surgery, which is some cases may involve amputating the leg or performing a heart transplant.
CONCLUSION
One researcher concluded: “We found that smoking was the single most important risk factor for the development of postoperative complications” (Moller, 2002).